
Pharmacological effects of fucoidan
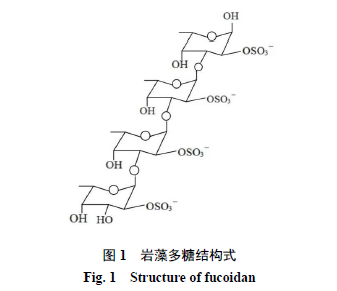
Fucoidan is a type of natural sulfated heteropolysaccharide isolated from the cell walls and intercellular matrix of brown algae [1]. Its structure includes a core skeleton composed of L-fucose and sulfate groups, as well as branched structures composed of glucose, galactose, xylose, mannose and glucuronic acid residues [2] (Figure 1). These structures serve as the supporting structure and "hydrophilic coating" of the cell wall, which can not only keep the cell in a moist environment, but also resist the damage to the algae caused by excessive light [3]. With the deepening of research, fucoidan has a variety of biological activities due to its rich sulfate groups and unique polysaccharide structure, such as anti-inflammatory, antitumor, neuroprotective, anticoagulant, intestinal flora regulation, blood lipid regulation, and antiviral effects. Therefore, this article summarizes the pharmacological effects of fucoidan in order to provide a reference for further development and utilization of fucoidan.
1. Anti-inflammatory
In asthma, its immune mechanism is closely related to helper T cells (Th). Among them, Th1 cells can secrete interferon-gamma (IFN-γ), and Th2 cells can secrete interleukin (IL)-4 and IL-10[4]. Th1 cells can inhibit the differentiation of Th2 cells and effectively reduce Th2-induced asthmatic response, but excessive release of IFN-γ by Th1 cells can also cause airway inflammation. Therefore, the imbalance of the Th1/Th2 ratio is considered to play a key role in the inflammatory response of asthma. In a clinical trial, 30 asthmatic patients and 15 healthy patients were recruited, and their peripheral blood mononuclear cells were collected. After treatment with fucoidan (100 or 500 µg/mL) for 48 h, the secretion of Th1, Th2 cells and other inflammatory factors was detected[5]. The results showed that the proportion of Th1 cells and the level of IFN-γ in the asthma group were significantly lower than those in the healthy group. However, after treatment with fucoidan, the levels of Th1 cells and IFN-γ increased, but the increase was not significantly different between the two groups. The level of Th2 cells did not change, suggesting that fucoidan may improve the Th1/Th2 level by not excessively increasing the Th1 level, thereby reducing the occurrence of airway inflammation. One of the harms of secondhand smoke is a toxic aldehyde called acrolein, which is present in tobacco smoke and can upregulate the expression of mucin 5AC (MUC5AC) and inflammatory factors in the human bronchial epithelial cell line NCI-H5. Pokharel et al. [6] used 30 µg/mL fucoidan to reduce the expression of MUC5AC in NCI-H292 cells. The mechanism may be by downregulating the expression of MUC5AC mRNA in NCI-H292 cells stimulated by acrolein, while inhibiting the activation of activator protein 1 (AP-1) on which the expression of MUC5AC depends. Ni et al. [7] treated RAW1.6 macrophages with 3.125, 6.25, 12.5, and 25 μg/mL fucoidan for 1 h, and then stimulated them with 1 μg/mL lipopolysaccharide (LPS) for 24 h to establish an inflammatory response. The results showed that fucoidan did not affect the proliferation activity of macrophages. LPS stimulation caused an excessive increase in the levels of inflammatory factors such as nitric oxide (NO), tumor necrosis factor-α (TNF-α), IL-1β, and IL-6 in macrophages, inducing an inflammatory response. Fucoidan significantly reduced the production of inflammatory factors in a dose-related manner, suggesting that fucoidan has a good inhibitory effect on the expression of pro-inflammatory cytokines in the LPS-induced inflammatory response of RAW 264.7 cells. For respiratory tract inflammation, the use of a lung delivery system with particulate drug carriers is a current method for treating airway diseases such as asthma, pulmonary infection, and chronic obstructive pulmonary disease. Fucoidan itself has good anti-inflammatory activity. If it can be combined with nanoparticles and loaded with conventional anti-inflammatory and bronchodilator drugs, and administered by nebulization, it can not only reduce the dosage of conventional drugs, but also improve the local bioavailability of fucoidan and effectively inhibit airway inflammatory response. In addition to its unique anti-inflammatory effect in respiratory tract inflammation, fucoidan can also reduce oxidative stress and inflammatory response in inflammatory bowel disease. Ahmad et al. [8] fed mice with sodium dextran sulfate to establish a mouse model of inflammatory bowel disease. The experimental group was treated with fucoidan 400 mg/kg for 7 days. It was found that compared with the control group mice, the levels of reactive oxygen species (ROS) and inflammatory factors IL-1β, IL-3, IL-6, IL-9 and TNF-α in the experimental group mice were significantly reduced, and the pathological scores of the overall tissues were improved. In an experiment targeting an inflammatory injury model of human colonic epithelial cells (NCM460), fucose at concentrations of 50, 100, and 200 μg/L for 24 h significantly reduced the expression of inflammatory factors IL-6 and TNF-α generated by LPS stimulation, and the effect was concentration-dependent. This effect may be related to the intervention of the Notch-1 signaling pathway [9]. In summary, fucose has been shown to have certain anti-inflammatory effects in both in vitro cell and animal experiments. However, the pathways involved in different diseases vary, and the effective intervention dose range and adverse reactions are not yet clear, which warrants further in-depth research and exploration.
2. Anti-tumor therapy
Cancer is a serious disease affecting human health, with high mortality rates and poor prognoses. Multiple courses of radiotherapy and chemotherapy drugs have significant adverse reactions, which are often difficult for patients to tolerate, while expensive targeted drugs impose a huge economic burden on patients. Therefore, finding drugs that can assist in cancer suppression and reduce treatment duration, or natural anti-cancer drugs with fewer adverse reactions, is one approach to cancer treatment. Fucoidan, as a marine-derived component, plays a role in assisting cancer suppression. Cysteine-aspartate-specific protease-3 (caspase-3) is an irreplaceable protease in apoptosis; one of the anti-cancer mechanisms of the commonly used chemotherapy drug cisplatin is the stimulation of caspase-3 activation and the induction of DNA damage in cancer cells. When cisplatin (5 μmol/L) was used to treat LLC1 lung cancer cells for 24 h, followed by treatment with 6.25, 12.5, 25, and 50 μg/mL fucoidan for 48 h, the decrease in cancer cell viability was more pronounced compared to the cisplatin-only treatment group, with the 50 μg/mL group showing the most significant effect. The mechanism was related to the promotion of caspase-3 activation [10]. In C57BL/6 mice transplanted with Lewis lung cancer, after 21 days of treatment with cisplatin combined with fucoidan, the tumor volume was smaller than that of the cisplatin-only treatment group and the fucoidan-only treatment group, indicating that the anticancer effect of cisplatin combined with fucoidan was greater than that of single-drug treatment [10]. Intervening in the growth cycle of cancer cells, upregulating pro-apoptotic proteins, or downregulating anti-apoptotic proteins are also methods of cancer suppression. When fucose (50, 100 μg/mL) was used to treat colon cancer cells HT29 for 24 h, the division of cancer cells was stopped in the G0/G1 phase, and the effect was more obvious in the 100 μg/mL group [11]. This effect may be related to the activation of the protein kinase B (Akt) signaling pathway. Arumugam et al. [12] treated liver cancer HepG-2 cells with 500 μg/mL fucose for 48 h and found that it could arrest the cell cycle in the G1 phase and significantly inhibit cancer cell proliferation, showing good anti-cancer activity. Zhang et al. [13] treated breast cancer MDA-MB-1 and MCF-231 cells with 200 μg/mL fucose for 48 h and found that compared with the control group, the expression of anti-apoptotic proteins Bcl-xL and Mcl-7 in the experimental group decreased, while the expression of apoptotic protein Bax increased, thereby inhibiting cancer cell proliferation. In addition to their unlimited proliferative capacity, the malignancy of tumor cells is also reflected in their strong invasive ability. Tumor cells achieve metastasis by destroying surrounding tissues and infiltrating normal cells. The ability of tumor cells to migrate is related to the expression of matrix metalloproteinases (MMPs). MMPs participate in the decomposition of the extracellular matrix (ECM) and assist cancer cells in invading surrounding tissues [14]. Lee et al. [15] found in an in vitro cell study that after treating lung cancer A549 cells with 50, 100, and 200 μg/mL fucoidan for 48 h, the activity of MMP-2 decreased by 36%, 53%, and 72%, respectively, and the inhibition rates of cancer cell migration in the corresponding groups were 25%, 46%, and 57%, respectively. This indicates that fucoidan can inhibit cancer cell migration by reducing the expression of MMP-2. The anti-cancer dose of fucoidan is not consistent in different experiments, which may be related to the sensitivity of cancer cells and the different absorption and utilization of fucoidan. As a water-soluble compound, the oral bioavailability of fucoidan may be reduced by the acidic environment of the stomach, so improving the utilization rate of the drug is extremely important. Pinheiro et al. [16] found that by using chitosan nanomaterials to encapsulate fucoidan, the effect of the gastric acidic environment on the polysaccharide can be reduced, which may be one of the prospective drug delivery methods for water-soluble compounds. In a xenograft osteosarcoma mouse model, the experimental group mice were ig 100 mg/kg nano-fucose polysaccharide particles for 28 days, while the control group mice were treated with water only. Compared with the control group, the tumor volume of the experimental group mice was significantly reduced, indicating that the nano-fucose polysaccharide particles have higher biological activity and excellent bioavailability, and are more effective than oral fucoidan [17]. Pawar et al. [18] electrostatically assembled fucoidan with cationic polyethyleneimine, loaded the anticancer drug doxorubicin, and formed immunotherapy nanoparticles. They treated tumor-bearing BALB/c mice for 26 days (loaded with doxorubicin 4 mg/kg). Compared with treatment with doxorubicin alone or fucoidan, the nanoparticles showed stronger antitumor effects. In addition, cancer often leads to a decrease in the body's resistance, making it easy to experience joint inflammation, pain, fever and other discomfort symptoms, which affect the quality of life of patients. In a prospective clinical study in Japan, 20 patients with advanced metastatic cancer were given 400 mL of fucoidan (10 mg/mL fucoidan) orally every day for at least 4 weeks. Compared with before treatment, the levels of pro-inflammatory factors such as IL-6 and IL-1β in the patients were significantly reduced after treatment, and their joint pain was also reduced [19]. In summary, fucoidan may not only be used as an adjunct anticancer drug, but may also be used as a medicinal diet to improve the quality of life of patients with advanced cancer.
3. Neuroprotection
Neuronal damage in the brain is most common in ischemic stroke, which causes hypoxia/glucose/reperfusion (OGD/RP) injury, which is the main cause of long-term disability in patients. Before establishing a rat PC12 cell OGD/RP model, some researchers treated the cells with 1 μmol/L fucoidan for 24 h. The experiment found that OGD/RP inhibited cell viability, increased intracellular ROS levels and promoted PC12 cell apoptosis. Compared with the control group, the ROS level in the fucoidan pretreatment group was significantly reduced, and the expression levels of superoxide dismutase (SOD) and glutathione peroxidase (GSH-Px), which have the effect of preventing oxidative stress, were significantly increased. This indicates that fucoidan can protect neurons from OGD/RP damage by inhibiting cell apoptosis and promoting the expression of antioxidant enzymes, which may be related to the inhibition of the JAK/STAT signaling pathway [20]. In a transient ischemic attack model, Kim et al. [21] pre-iped fucoidan 25 mg/kg, once a day, for 5 days. The results showed that the fucoidan pretreatment group could effectively inhibit the activation of astrocytes and microglia in ischemic areas, reduce the production of superoxide anion free radicals, and significantly increase the expression of SOD. This indicates that fucoidan can reduce oxidative stress by weakening activated glial cells and increasing the production of SOD, thereby effectively protecting neurons from the effects of ischemic events. Alzheimer's disease is the most common type of dementia. One of its pathological features is the accumulation of extracellular senile plaques, the main component of which is amyloid protein, which is toxic to neurons. In in vitro experiments of Alzheimer's disease, PC12 neurons were treated with 100 μg/mL fucoidan for 24 h and it was found that it could inhibit the formation of amyloid protein and its toxic effect on neurons [22]. In addition to its protective effect on brain neurons, fucoidan also has an ameliorative effect on peripheral nerves. Diabetic patients are prone to peripheral nerve dysfunction due to poor long-term blood sugar control, which can lead to conditions such as limb numbness and decreased taste sensitivity. In one clinical trial, patients with diabetes were given 60 mL of fucoidan (containing approximately 1,620 mg of fucoidan) orally daily for 12 weeks on top of their routine treatment. The results showed that the thresholds for sweet, salty, bitter, and umami tastes in these patients were significantly lower than before treatment (increased sensitivity), indicating that fucoidan can improve peripheral neuropathy caused by long-term hyperglycemia to some extent [23]. It is evident that fucoidan can be further developed as a neuroprotective drug, but its effectiveness in protecting brain nerves still needs further validation, mainly due to the challenge of penetrating the blood-brain barrier in in vivo experiments. Currently, there is a lack of research on penetrating the blood-brain barrier. In the future, further in-depth research on the delivery system of fucoidan may be needed to increase its penetrability and prolong its half-life, which may help it play a better role.
4.Anticoagulation
Thrombolysis via intravenous injection of recombinant tissue plasminogen activator (rtPA) is the most common interventional treatment for recanalizing blood vessels blocked by acute thrombosis. However, rtPA is rapidly neutralized by circulating PA inhibitor-1 (PAI-1) after intravenous administration, reducing its efficacy. Therefore, blocking the inhibitory pathway or directly increasing free rtPA can lead to enhanced thrombolysis. In a joint study, it was found that in a mouse model with thrombus occlusion for 30 min, fucose 100 mg/kg was injected into the tail vein in addition to routine thrombolytic therapy. After 3 h of observation, the fucose group was able to dissociate the rtPA/PAI-1 complex, release free rtPA, and exert a better thrombolytic effect [24]. P-Selectin is a cell adhesion molecule expressed in activated endothelial cells and platelets, and fucose has a good affinity for P-Selectin expressed in activated platelets in thrombi. Fucoidan was incorporated into nanoparticles and rtPA was loaded simultaneously. The affinity between fucoidan and P-Selectin made the target thrombolytic drug more accurate [25]. Bonnard et al. [26] dissolved pullulan (9 g), dextran (3 g) and FITC-dextran (100 mg) in 40 mL of purified water and added 1.2 g of fucoidan to prepare a mixture, which was used to construct a new single-photon emission computed tomography (SPECT) diagnostic tool (composed of 99mTc and fucoidan). The experiment found that this mixture had a higher sensitivity to thrombus detection and more accurate localization when performing SPECT examination. Superparamagnetic iron oxide nanoparticles SPION coated with dextran are often used as MRI contrast agents, but SPION is easily removed from circulation through the reticuloendothelial system. When an appropriate amount of fucoidan is added, it can prevent SPION from being taken up into the reticuloendothelial system, prolonging the half-life of SPION from 37.4 min to 150 min, so that MRI examination can better detect aneurysm thrombosis or other vascular lesions [27]. In summary, fucoidan has a certain degree of amplification of anticoagulation effect, and appropriate concentrations of fucoidan combined with thromboangiography drugs can also help to better detect vascular thrombosis lesions. However, the concentration range of different effects of fucoidan needs to be further determined by experiments in order to reduce the occurrence of adverse reactions.
5.Regulation of gut microbiota
The gut of mammals is colonized with trillions of microorganisms. Under normal circumstances, the gut microbiota and the body's immune system are in a dynamic balance, which is beneficial to human health. However, when various factors are overstimulated, the number or types of microbiota may change significantly, the microecological balance is broken, the body's metabolism is disordered, and inflammation and related metabolic and immune diseases are promoted [28-29]. Therefore, by regulating these microorganisms, it may be possible to directly or indirectly assist in the digestion of complex dietary nutrients, resist pathogen infection, fight inflammation and maintain the immune system [30-31]. Studies have found that fucoidan also has the effect of regulating gut microbiota. Xue et al. [32] fed breast cancer rats 200 and 400 mg/kg of fucoidan every day for 16 weeks and observed the intestinal condition. The results showed that the gut microbiota ratio of breast cancer rats was imbalanced and the intestinal wall was damaged. When fucoidan was given, the composition of gut microbiota could be improved, thereby repairing the intestinal barrier function and gradually restoring the intestinal villi. The effect was more obvious in the 400 mg/kg group. Before the immunocompromised mouse model constructed with cyclophosphamide, mice were fed with fucoidan (50 mg/kg) daily for 28 days. The intestinal structure of the model group mice was severely damaged, and the excessive increase in Bacteroidetes content disrupted intestinal function. After the intervention of fucoidan, the disordered flora structure was greatly restored, especially the number of beneficial lactobacilli increased significantly, indicating that fucoidan can alleviate intestinal inflammation by regulating the structure of the intestinal flora [33]. Helicobacter pylori is a Gram-negative bacterium with a strong ability to survive in the harsh acidic environment of the stomach. Its infection often causes peptic ulcer disease. Studies have found that Helicobacter pylori infection can lead to intestinal flora disorder and even affect the treatment of the original disease [34]. In an animal experiment, mice were given 3 mL of 40 g/L fucoidan by ig daily for 2 weeks, and then 3 mL of Helicobacter pylori suspension by ig for the next 3 weeks to establish a Helicobacter pylori infection model. Analysis of mouse feces revealed that, compared with the untreated group, the intervention group showed a significant reduction in harmful bacteria and a significant increase in beneficial bacteria such as Bifidobacterium and Fatty Bacteria, indicating that fucoidan can regulate the intestinal flora disorder in Helicobacter pylori-infected mice [35]. The above results suggest that fucoidan has the function of regulating intestinal flora, but further research is needed to explore the possible mechanisms involved in this function and the degree of influence on different bacterial groups. This will be beneficial for its subsequent development into an intestinal microbial regulator or functional food.
6. Regulation of blood lipids
Blood lipids are essential substances for cellular basal metabolism, and their main components are total cholesterol (TC), low-density lipoprotein cholesterol (LDL-C) and triglycerides (TG). Under normal circumstances, blood lipids participate in human energy metabolism, but when blood lipid levels are abnormal, they become risk factors for diseases such as coronary heart disease, diabetes, stroke, and kidney disease, which are not conducive to the treatment of the original diseases. In an early lesion model of alcoholic liver disease in mice, 300 mg/kg of fucoidan was administered daily for 8 weeks. It was found that compared with the untreated group, the intervention group significantly reduced the serum TC, LDL-C, and TG levels in mice [36]. This indicates that fucoidan can improve the disorder of liver lipid metabolism in alcoholic liver disease and reduce liver lipid toxicity. Huang Jinli [37] established an obesity-related hyperlipidemia model by feeding mice a high-fat diet. The intervention group was given 50 and 250 mg/kg of fucoidan daily for 5 weeks. The results showed that compared with the model group, the mice in the intervention group had a reduced increase in body weight and significantly improved levels of TC, TG, and LDL-C. The effect was more obvious in the 250 mg/kg fucoidan group. This indicates that fucoidan can improve obesity-related hyperlipidemia. Eo et al. [38] fed a hyperlipidemic mouse model 250 mg/kg of fucoidan 5 times a week for 12 weeks. The results showed that compared with the control group, fucoidan intervention could significantly reduce the adipose tissue mass, blood lipids, and liver fat deposition induced by a high-fat diet. The above results indicate that fucoidan has the potential to be developed into a lipid-regulating functional food, but large-sample data are still needed to evaluate the concentration range of its effect.
7. Antiviral effects
Fucoidan also has a certain effect on antiviral activity. Influenza A virus is a common respiratory pathogen with high infectivity. It has caused a pandemic and harmed health [39]. Therefore, developing new, low-toxicity anti-influenza A virus drugs is one of the ways to treat it. Wang et al. [40] used 31.25, 62.5, 125, and 250 μg/mL of fucoidan to intervene in A549 cells infected with influenza A virus. The results showed that when the fucoidan concentration was greater than 62.5 μg/mL, it could significantly reduce the viral titer and increase cell viability. The effect was concentration-dependent. Human T-lymphotropic virus type 1 (HTLV-1) is a single-stranded RNA retrovirus that can cause HTLV-1-associated myelopathy/tropical spastic paraplegia (HAM/TSP) and adult T-cell leukemia (ATL) [41]. In a single-center, open-label trial, 13 HAM/TSP patients received 6 g of fucoidan daily for 6–13 months. Fucoidan reduced HTLV-1 viral load in cells by 4.1% without affecting host immune cells. These patients did not experience disease exacerbation during treatment [42]. Oral herpes is often associated with herpesvirus infection. Creams containing 4% fucoidan also have excellent inhibitory activity against herpesvirus and can effectively treat oral herpes [43].
8. Conclusion and Outlook
Fucoidan's broad-spectrum bioactivity allows it to be used not only as a standalone drug but also as an adjuvant in various drug formulations. When combined with nanoparticles and liposomes to develop drug carriers, it can not only protect the activity of the loaded drug but also increase its utilization and improve therapeutic efficacy. While marine-derived components have advantages such as naturalness and uniqueness, they also have some drawbacks. First, marine pollution can affect the species from which fucoidan is derived, resulting in poor-quality extracted fucoidan. This problem can be addressed by artificially simulating large-scale cultivation of brown algae in a marine environment, but the bioactivity of fucoidan extracted from artificially cultivated brown algae needs to be demonstrated. Second, although fucoidan can function as an adjuvant, the specific drug interactions between fucoidan and anti-tumor drugs, anti-inflammatory drugs, etc., are still unclear and require further research. Finally, the commercialization of fucoidan is not easy. Although it has demonstrated broad bioactivity in experiments, its adverse reactions and harmful dosage as a drug are not fully understood, and regulatory authorities will strengthen the supervision of this type of drug to prevent its widespread use. In conclusion, fucoidan, as a marine-derived component with broad bioactivity, will play a greater role in the medical and pharmaceutical industries, and more experimental studies are needed to explore its mechanisms of action in various treatments.
References (omitted)
Source: Tang Huanhuan, Li Qi, Zhou Xiangdong. Research progress on the pharmacological effects of fucoidan [J]. Modern Drugs and Clinical, 2023, 38(7):1786-1793.
